Patients with 5 or more miscarriages have an outstanding 70% chance of having a baby using their own egg and our treatment protocols.
Posted By Braverman IVF & Reproductive Immunology || 30-Jan-2018
A review of 76 cases at Braverman IVF & Reproductive Immunology
Under our care almost 70 % (52/76) of our patients, with a history of reccurent pregnancy loss (RPL) and a minimum of five miscarriages, have had at least one successful pregnancy using their own egg (Figure 1) as defined by a live birth (***, p< .0009). (A low p value such as this shows a very high statistical significance).
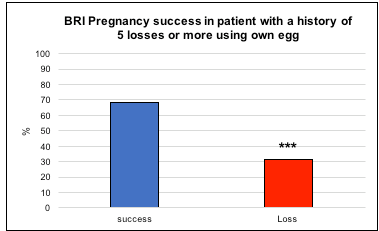
Figure 1: Overall pregnancy success at Braverman Reproductive Immunology in patient with a history of RPL and a minimum of 5 losses using their own egg.
•70% of the documented losses were aneuploid (abnormal) which shows that our therapies are effective in maintaining euploid pregnancies.
No significant difference was determined between the types of infertility as shown in Figure 2.
- Primary has no history of a successful birth prior to the miscarriages
- Secondary has a history of a full-term birth followed by miscarriages
- Tertiary has a history of miscarriages prior to and after a full-term birth.
Figure 2: BRI pregnancy success rate based on type of infertility in patient with a history of 5 losses or more and using their own egg.
Our high pregnancy success rate is maintained and even further increased in older patients as seen by an exceptional success rate of over 90% in patient aged 41-42-year-old.
Figure 3: BRI pregnancy success rate based on age at conception in patient with a history of 5 losses or more and using their own egg in addition to our therapy protocols.
• If we now consider patients with a history of at least 5 losses and requiring donor oocytes (excluded from the analysis in the Figure 1-3 above), 50% had at least one loss prior to our care with donor egg despite a good quality embryo (donor was less than 35 years old) while the other half went on with a donor egg cycle after multiple miscarriages using their own eggs.
• But under our care, 83% of them had a successful pregnancy at the first attempt (5/6), while 17% were not after one single attempt (1/6).
By providing our patients adjusted and adequate therapies, these women are now already happy mothers.
The most important aspect in deciding to treat patients with a history of recurrent miscarriage is to understand their risk of further miscarriages when no treatment is offered. To this end the literature appears abundantly clear.
1. Women with a history of miscarriage and whose pregnancy was proven genetically normal (by testing of the Products of Conception or by PGS tested embryos) have a significantly greater risk for further miscarriages.
2. Women with documented losses where the Products of Conception were genetically abnormal do not appear to be at risk for further miscarriages.
3. Women with a history of miscarriage which were proven genetically normal still have an increased risk for further miscarriages, even if they have another loss that is proven to be genetically abnormal.
4. Women who have a miscarriage where the genetics were not able to be tested, have a high likelihood that the pregnancy was genetically normal and therefore they are at increased risks for future miscarriages if:
a. There waspresence and loss of a fetal heart beat (this becomes more significant the further along the pregnancy goes).
b. Those with a history of 5 or more miscarriages
c. Those patients that miscarry with donor embryos from a young donor (< 35-year-old)
d. Multiple losses in a young woman (under age 35 with no history of abnormal karyotype i.e. the mother or father do not have genetic abnormalities)
5. Treating any group of patients where there is no clinical history of genetically normal (euploid) losses should offer no benefit as the losses in this group of patients would therefore, most likely, be genetically abnormal (aneuploid) and the literature shows that aneuploid losses are not predictive of further miscarriages, i.e. most of these patients would succeed without treatment.
To this end then it also is true that any study looking at the risk of future miscarriages that includes as its majority a patient population with mostly aneuploid losses (chemical pregnancies, loss prior to fetal heart rate, or of course abnormal genetic testing of the products of conception) will have an artificially high rate of success with subsequent (future) pregnancies (i.e. if the aneuploid pregnancy does not increase risk for another loss then these patients have a good chance of pregnancy without treatment).
At the time much of the literature predicting future success in the recurrent pregnancy loss population was written, many of these issues were not addressed, leading to misunderstand and therefore misinterpretation of predicted success rates in women with recurrent pregnancy loss where no medical therapy was initiated.
It also holds true that evidence of treatment success in the group of women at risk for further miscarriages (those with history of euploid loss) should show:
• a decrease in the number of euploid losses (over the predicted rate without treatment) once therapy is initiated i.e. most of the losses should be aneuploid as these would not benefit from treatment
• And of course, an increase in the successful pregnancy outcome rate.
With this in mind we begin a review of the literature that attempts to define the chances of success after a history of recurrent pregnancy loss, then we will discuss our success rate in a group of well-defined at risk patients and compare this with the known literature.
1. The Brigham study: the reference to date in establishing outcome of a subsequent pregnancy in RPL patients
One of the first studies focusing on RPL patients and subsequent pregnancy losses was published in 1999 in the Journal of Human Reproduction (1) and remains to date the most quoted study focusing on recurrent miscarriages. They unknowingly excluded most of the patients that would have “euploid” losses, leaving them with mostly a population of patients that were having aneuploid losses, which we now understand do not have an increased risk of reoccurrence. Calculations of success after any number of miscarriages in this group of patients would therefore be artificially elevated.
• They excluded all the below patients: all high risk for “euploid” losses.
- Anti-Phospholipid antibodies (this would therefore eliminate many with autoimmune diseases and silent endometriosis)
- Oligomenorrhoea, light or infrequent cycle, (this would eliminate many with PCOS, and those with rising FSH levels, another indicator for silent endometriosis)
- Endocrine abnormalities
- Known Endometriosis
• Patients with a history of second trimester loss (euploid loss)
• They failed to document the time of first positive βhCG with their next pregnancies (patients came to the clinic when they wanted, so many of the biochemical pregnancies in the study population were likely missed). Many patients who were pregnant but had a “late” bleed most likely never came in and these losses were not recorded.This would artificially lower the number of miscarriages in the study and therefore artificially elevate the successful pregnancy rates.
• There is no timeline in women’s enrollment into the study, they presented spontaneously (when they wanted to) and 10% of patients presented after 8 weeks, at a time when miscarriages are less likely to happen.
As a result, the study is biased, as seen by the majority of aneuploid losses (89%) while only 11% of fetal losses occurred with a fetal heartbeat detected at the time of loss so most likely euploid. If this was a group at high risk for repetitive losses, most of the losses in this untreated group would have been euploid.
Therefore, this population group is not at increased risk for a subsequent pregnancy and are more likely to have a future pregnancy success with no treatment.
2. Recurrent pregnancy loss patients have a higher risk of future euploid losses
a- Literature Review
Ogasawara and collaborators (2) showed that the likelihood of a loss being normal (euploid) was higher in recurrent miscarriage patients (48.7%) compared to the control population of those having a miscarriage for the first time (23.7%). Only 35% of RPL patients in this study managed to have a successful pregnancy, with treatment (compared to 70% for our patients here at Braverman Reproductive Immunology with treatment).
Interestingly, the frequency of an aneuploid (abnormal) loss significantly decreased with the number of previous miscarriages, while that of a normal loss (euploid) significantly increased (showing that those with high number of miscarriages were most likely losing euploid pregnancies and that these types of losses tend to reoccur without treatment).
These results were confirmed by another team led by Morikawa (3) showing that RPL patients are more prone to have another euploid loss. In this study, euploid losses were shown to be significantly higher in RPL patients (66.7%) vs. controls (45.7%) while aneuploid losses remain the same between the two groups. Again, showing that it is the euploid losses that most likely need treatment.
In this study, 49% of patients had a successful pregnancy with treatment, compared to 70% on our patients here at Braverman IVF & Reproductive Immunology.
Another study by Carp and collaborators (4) focused on genetic testing on products of conception in patients with 3 or more miscarriages.
They found that the incidence of aneuploid losses among these miscarriages was 29% while 71% of losses were euploid. They also estimated that after an aneuploid loss, 68% will have a live birth while only 41% will have a live birth after euploid losses.
Altogether these studies showed that:
• RPL patients are more prone to have another miscarriage that is documented as a euploid loss
• this risk increases with the number of miscarriages (showing that higher number of miscarriages is more likely to be associated with euploid losses)
b- Success treating RPL patients with history of euploid losses: the Ogasawara study
In their study, Ogasawara and collaborators included a large set of patients with RPL (n=1309) who had between 2 and 20 consecutive first trimester losses before a subsequent pregnancy (2). Unlike Brigham’s work, his study design included:
• Autoimmune disease: Anti-phospholipid syndrome, diabetes, hyperthyroidism
• Oligomenorrhoea (light or infrequent cycle)
• Endocrine abnormalities: PCOS
• Known Endometriosis cases
• All patients with a history of at least 2 losses regardless of the time of the loss (first or second trimester) were also included
• They also included all the patients whose first beta HCG was drawn 2 weeks after conception (i.e. 4 weeks of pregnancy) so the biochemical pregnancies were all included.
Immune therapy was administrated to patients with at least 3 prior pregnancy losses. In this study, they reported on patients with 5 or more previous miscarriages, and their success rate was 35% despite immune therapy (compared to 70% in our patients). The authors acknowledged the fact that the treatments provided are somehow not really adapted and/or inefficient as:
• The pregnancy success rate should have been higher if the therapy was appropriate
• There should have been fewer euploid losses (70% in their study). At Braverman Reproductive Immunology, only 30% of the tested Products of Conception were euploid, 70% were aneuploid showing a significant success in maintaining euploid pregnancies with treatment.
3- Pregnancy success with Braverman Reproductive Immunology (BRI)
a- What are my chances with Braverman Reproductive Immunology?
Because the number of miscarriages directly impacts pregnancy success, we have chosen to focus on women with 5 or more losses (N=76 cases) who have statistically lower chances of having a successful pregnancy. The average age of RPL women when coming to us was 37.5 years (27-44 years), with an average of 7 pregnancy losses (from 5 to 15 losses). Unlike the Brigham study, we included all patients regardless of their medical history (PCOS, endometriosis, autoimmune diseases etc…) as well as biochemical pregnancies preventing us from underestimating our pregnancy loss rate. Prior to conception, all RPL women had been subjected to examination by ultrasonography and hysterosalpingography to detect anatomical abnormalities of the genital tract or cervical incompetency. All our patients underwent our unique extensive genetic and immunologic panel screening including:
• Genetic testing: full HLA profile to determine the compatibility between couple and define predisposition for immune diseases that could explain immune alterations
• Cellular testing that looks at cell numbers and their propensity to make certain cytokines which allow us to determine how the immune system is pointing (Th1 or Th2 dominant state)
• Serum cytokines and antibodies quantification to determine the level of activity of the immune system
Patients received appropriate therapy before conception (natural conception or IVF cycle) and the treatment was maintained at least throughout the first trimester of pregnancy.
• Prior to our care, 95% of our patients (with documented history of their prior losses) had at least one euploid loss compared to 11% in the Brigham study.
The high level of euploid losses suggest that immune defects could be responsible for those pregnancy losses.
• Under our care, almost 70% of our patients had a successful pregnancy.
b- Where do we stand in comparison with other studies?
Despite an increased risk of pregnancy losses due to the higher number of previous miscarriages and the different pathologies affecting our population group (autoimmune diseases, PCOS, endometriosis) compared to the other studies, we did get the highest rate of pregnancy success with an outstanding 70% success. In the Birgham study, the pregnancy success rate was 52.15% but largely overestimated due to the possible missed embryonic losses as patients presented to the clinic by 8 weeks and not right after a positive βhCG test. Furthermore, as seen by the high percentage of aneuploid losses (89%), they selected a population that was shown to have a lower risk for further miscarriages. Ogasawara study is very reliable and comparable to our work in term of inclusion/exclusion criteria but failed to get a higher rate of pregnancy success despite the use of immune therapy (35% success). As stated by the authors, this showed that “therapeutic approaches are not sufficiently efficacious”
Besides our outstanding pregnancy success rate (70%) with the use of an adjusted therapy regimen, it is important to underline that only 30% of the documented losses were euploid.
Although not every sample was able to be tested, the fact that 30% of the tested samples showed a euploid loss is very significant and shows that our immune therapies are highly effective in retaining euploid pregnancies.
We, at Braverman IVF & Reproductive Immunology, keep working in improving our pregnancy success rate by developing new tests to detect immune parameters potentially affecting the establishment and maintenance of pregnancy. By offering custom-designed strategies to counteract the detrimental effects of certain factors, we hope to exponentially help women to become mothers.
References